GIT Transit Time & SIBO: Accurate Testing Starts with Timing
What is GI transit time? Gastrointestinal (GI) transit time is the duration required for ingested material to pass through the digestive tract from...
2 min read
![]() Dr. Andrea Gruszecki, ND
:
February 8, 2021 at 2:05 PM
Dr. Andrea Gruszecki, ND
:
February 8, 2021 at 2:05 PM

February is American Heart Month and is the perfect opportunity to consider our cardiovascular health. One measure of cardiovascular risk is total IgE. Several human studies have documented higher total IgE as a cardiovascular risk factor after adjusting for “classic” risk factors such as smoking, fasting glucose, blood pressure, LDL-cholesterol, etc. (Criqui; Kovanen; Min). However, a more recent large population study concludes that the presence of allergic rhinitis (“hayfever”), known to raise IgE levels, may be protective (Crans Yoon). How do we fit these puzzle pieces fit together?
These contradictory findings begin to make sense if we look more closely. Total IgE reflects all of the IgE antibodies in circulation. An individual can make IgE antibodies to aeroallergens (pollens, molds, etc.) or foods:
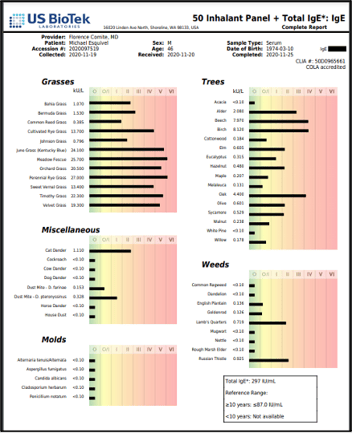
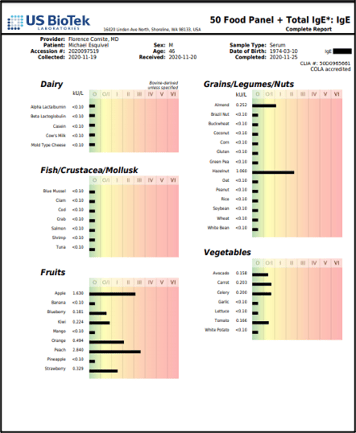
[Total IgE 297 IU/mL Reference Range 10 years-adult: < 87.0 IU/mL]
Or, IgE can be high in the absence of pollen or food allergies:
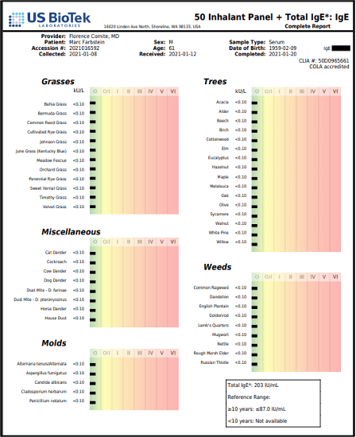
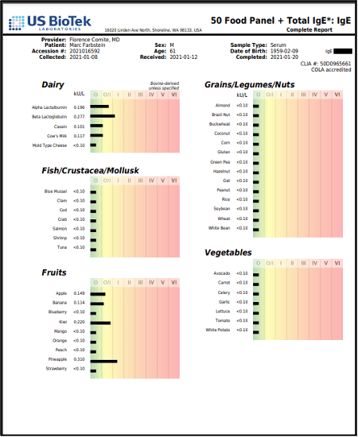
[Total IgE 203 IU/mL Reference Range 10 years-adult: < 87.0 IU/mL]
Studies indicate that autoimmune IgE reactions are often to blame, and that IgE-mediated autoimmunity against proteins in blood vessels, cardiac tissues or blood lipids may be responsible for the higher total IgE readings. So, a higher IgE associated with plant foods or plant aeroallergens means fewer IgE autoantibodies and lower overall cardiovascular risk (Crans Yooon; Xu). Of note, one large population study discovered that a higher total IgE, in association with dust mite-specific antibodies, did increase the risk of angina and concluded that assessing both total and antigen-specific IgE was more clinically useful than just total IgE (Xu).
The binding of IgE to mast cells, basophils or macrophage precursors (monocytes) induces the release of histamine and a variety of proinflammatory mediators, such as thromboxanes, leukotrienes, and tryptase. All of these proinflammatory molecules contribute to the development of atherosclerotic plaques in blood vessels. The build-up of plaque narrows the artery lumen, and hardens the artery raising blood pressure and decreasing blood flow. Poor circulation starves the heart and other tissues of essential oxygen and other nutrients, predisposing the cells to mitochondrial dysfunction and chronic inflammation (Madamanchi).
The five leading preventable risk factors for CVDs are hypercholesterolemia, diabetes, hypertension, obesity and smoking. Higher total IgE is another cardiovascular risk factor that can easily be assessed and monitored. Suppression of allergy symptoms with nasal glucocorticoids and oral antihistamines was shown to reduce both high blood pressure and systemic inflammation (hs-CRP) in a human study (Magen). These results indicate that naturopathic and functional medicine may have much to offer patients with higher total IgE and cardiovascular risks, with fewer side effects:
References:
Crans Yoon AM, Chiu V, Rana JS, Sheikh J. Association of allergic rhinitis, coronary heart disease, cerebrovascular disease, and all-cause mortality. Ann Allergy Asthma Immunol. 2016 Oct;117(4):359-364.e1.
Criqui MH, Lee ER, Hamburger RN, Klauber MR, Coughlin SS. IgE and cardiovascular disease. Results from a population-based study. The American Journal of Medicine. 1987 May;82(5):964-968.
Kovanen PT, Mänttäri M, Palosuo T, Manninen V, Aho K. Prediction of myocardial infarction in dyslipidemic men by elevated levels of immunoglobulin classes A, E, and G, but not M. Arch Intern Med. 1998 Jul 13;158(13):1434-9.
Madamanchi NR, Runge MS. Mitochondrial dysfunction in atherosclerosis. Circ Res. 2007 Mar 2;100(4):460-73.
Magen E, Yosefy C, Viskoper RJ, Mishal J. Treatment of allergic rhinitis can improve blood pressure control. J Hum Hypertens. 2006 Nov;20(11):888-93.
Min KB, Min JY. Risk of Cardiovascular Mortality in Relation to Increased Total Serum IgE Levels in Older Adults: A Population-Based Cohort Study. Int J Environ Res Public Health. 2019;16(22):4350.

What is GI transit time? Gastrointestinal (GI) transit time is the duration required for ingested material to pass through the digestive tract from...
Overview Many clinicians searching for answers about mycotoxin testing ask questions like “Should I provoke mycotoxins before urine testing?”, “When...

US BioTek Laboratories today announced the completion of its merger with NutriPATH Pathology, a respected functional pathology laboratory serving...