GIT Transit Time & SIBO: Accurate Testing Starts with Timing
What is GI transit time? Gastrointestinal (GI) transit time is the duration required for ingested material to pass through the digestive tract from...
2 min read
![]() Dr. Andrea Gruszecki, ND
:
December 9, 2020 at 9:42 AM
Dr. Andrea Gruszecki, ND
:
December 9, 2020 at 9:42 AM

There is no one “perfect” diet for everyone. After the dietary indulgence that often accompanies the December holidays, many of our patients will resolve to “get healthy” for their New Year’s resolution. A quick internet search will provide a dizzying array of dietary advice, much of which has little scientific support. Our patients may then turn to us for advice – what will we tell them?
If we are wise, we will tell them that everyone uses their macronutrients (proteins, carbohydrates and fats) differently. Some patients may flourish on a Mediterranean diet, others will do well with a Paleo-type diet, and still others may require a “keto” diet.
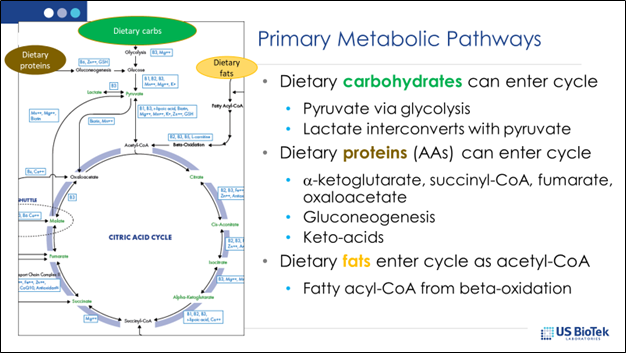
Before recommending a specific type of diet, it may be best to find out how well that individual patient can handle proteins, carbohydrates and fats, so that a personalized diet and supplement schedule can be designed to support their use of dietary macronutrients. A dried urine Organic Acids test can evaluate not only a patient’s use of macronutrients, but can provide suggestions for additional nutritional support so that the patient can better assimilate those nutrients and use them to generate ATP energy for their bodies.
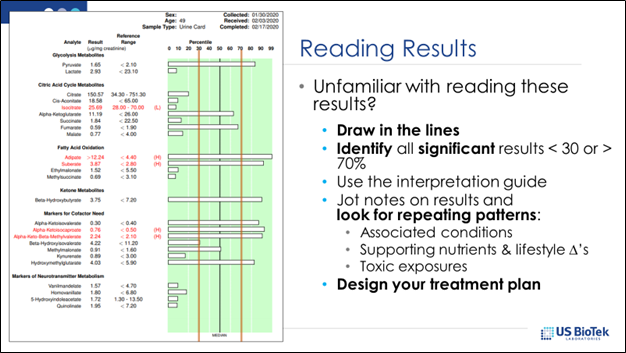
As seen in the above illustration, all three types of macronutrients are meant to eventually funnel into the citric acid cycle (CAC). However, due to inheritance, malnutrition or environmental exposures, the enzyme pathways meant to channel macronutrients into the CAC may be inhibited. It is these enzyme inhibitions that determine which macronutrient ratios and nutritional supports will work best for each patient. It is important to remember, when reviewing Organic Acids results, that the 50% is the top of the bell-shaped curve, and that results below 30% or above 70% require attention and support:
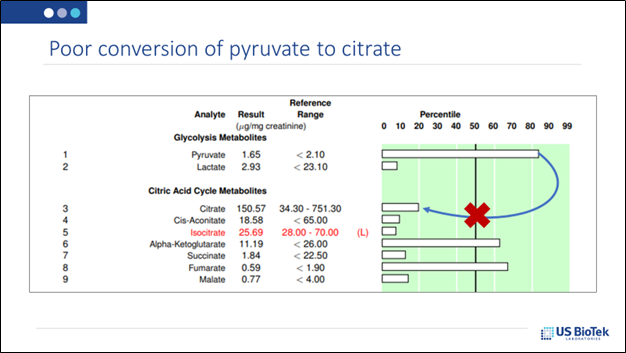
Using the 30-70% guideline, it is easy to determine which patients cannot easily convert carbohydrates (via glycolysis) into pyruvate and ultimately, citrate. These patients may develop high blood sugar if they are on a carbohydrate-heavy diet long-term.
Not familiar with these biochemical pathways? Download the US BioTek “Organic Acids in Central Energy Pathways” Chart and follow along!
Other patients may have trouble converting both carbohydrates (via glycolysis) and proteins (via gluconeogenesis) into pyruvate. If they have additional inhibitions preventing the conversion of lactate into pyruvate, then the CAC will starve unless building blocks are provided from another dietary source: fats.
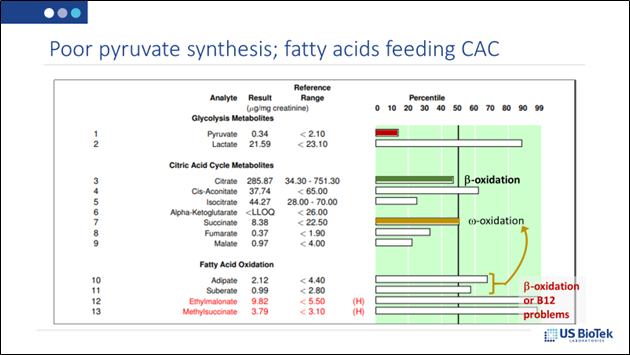
With additional nutritional supports (B12, etc.) as indicated by the Organic Acids Profile the patient illustrated above may thrive with a higher percentage of fat in their diet.
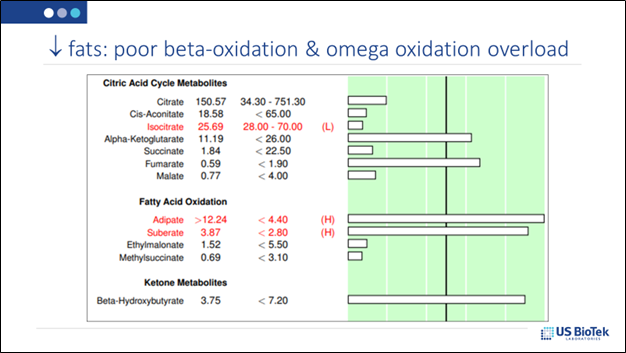
However, not everyone can handle a high-fat diet or a high-protein diet. Some of these metabolites, at very high levels can inhibit mitochondrial functions and other primary biochemical pathways:
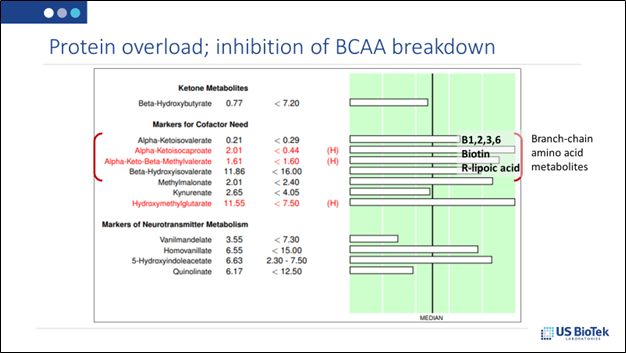
In conclusion:
We can see from the above examples that there is no one “perfect” diet for everyone. It is possible to give personalized diet and nutrition advice to each and every patient, based upon the function of their individual physiology. A patient-specific diet is the most likely to support the health and weight-loss goals that often accompany the New Year.
Watch More:
Berg JM, Tymoczko JL, Stryer L. (2002) Biochemistry, 5th edition. WH Freeman, New York, New York.
Esparham AE, Smith T, Belmont JM, et al. Nutritional and Metabolic Biomarkers in Autism Spectrum Disorders: An Exploratory Study. Integr Med (Encinitas). 2015;14(2):40-53.
Hernández-Aguilera A, Rull A, Rodríguez-Gallego E, et al. Mitochondrial dysfunction: a basic mechanism in inflammation-related non-communicable diseases and therapeutic opportunities. Mediators Inflamm. 2013;2013:135698.
Ramsay J, Morton J, Norris M, Kanungo S. Organic Acid Disorders. Ann Transl Med. 2018;6(24). DOI: 10.21037/atm.2018.12.39.
Wanders RJ, Komen J, Kemp S. Fatty acid omega‐oxidation as a rescue pathway for fatty acid oxidation disorders in humans. FEBS J. 2010. https://doi.org/10.1111/j.1742-4658.2010.07947.x .

What is GI transit time? Gastrointestinal (GI) transit time is the duration required for ingested material to pass through the digestive tract from...
Overview Many clinicians searching for answers about mycotoxin testing ask questions like “Should I provoke mycotoxins before urine testing?”, “When...

US BioTek Laboratories today announced the completion of its merger with NutriPATH Pathology, a respected functional pathology laboratory serving...