To Provoke, or Not To Provoke?: Mycotoxin Provocation Testing
Overview Many clinicians searching for answers about mycotoxin testing ask questions like “Should I provoke mycotoxins before urine testing?”, “When...
4 min read
![]() Dr. Andrea Gruszecki, ND
:
July 13, 2021 at 10:06 AM
Dr. Andrea Gruszecki, ND
:
July 13, 2021 at 10:06 AM

There are many different reasons for unexpected IgG results. Pre-analytical errors, which are outside of laboratory control, are responsible for the majority of our unexpected laboratory results.
Laboratory testing is an essential part of confirming a suspected diagnosis. Most experienced clinicians have a general sense of what to expect when they order laboratory testing, which is best expressed by the old saying “when you hear hoofbeats, expect horses, not zebras”. Yet, sometimes, when the lab results return, we see not only zebras but unicorns! Such “unicorns” are often caused by pre-analytical errors.
What is a pre-analytical error?
Multiple studies show that the greatest source of lab results error are events that occur before the sample ever reaches the lab. These are called preanalytical errors. US BioTek has created the VeriTekÔ process https://www.usbiotek.com/veritek , a rigorous quality control policy that ensures accurate, reproducible results. Yet, unexpected results still happen due to pre-analytical errors. Let’s take a look at a few common examples that can result in unexpected low IgG values:
Some of the most common pre-analytical errors encountered with IgG testing include
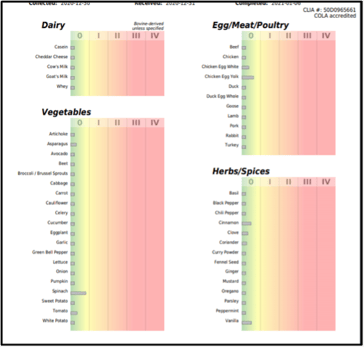
IgG antibody responses build up over a period of roughly 4 weeks, and have a half-life, once exposure stops, of about 25 days. This is why it takes a minimum of three months for IgG levels to decline post-exposure. This also means that, when testing IgG, a recent food exposure is required, unless such exposure risks an anaphylactic response. Ideally, the food would be brought back into the diet, 2 ounces daily for at least 2 weeks, and then could be discontinued while the immune response continues to develop for 2 weeks, then test. This protocol was specifically developed for Celiac testing, to minimize exposure but get a sufficient immune response for testing.
However, different foods are made up of a variety of different proteins, any one of which may instigate an immune response. Some of the proteins are more “universal” and shared across different species; these can results in food-food or pollen-food cross-reactions https://www.usbiotek.com/webinar/CrossReactivities-LookingBeyondFood . Each different food will have varying levels of these proteins, so that it may take a higher dose of one food and a lower dose of another to evoke an immune response in an individual.
While collection via fingerstick is convenient for many clinicians and their patients, it can also be a source of pre-analytical error. A good bloodspot sample requires free-flowing blood. If this cannot be achieved, then a serum sample is the best choice. US BioTek has partnered with several collection centers to facilitate the collection of serum samples https://www.usbiotek.com/blood-draw-locations .
Some patients will have poor peripheral blood flow, or other difficulties with the collection process and will end up excessively “milking” their fingers. These “milked” samples tend to be very low in IgG and often give the impression that the patient is clinically immunosuppressed.
In addition, fingerstick collections are contraindicated in very young children. If a child is less than 18 months old, a heel-stick collection (by an experienced collector) is indicated.
While a variety of medical conditions can result in low IgG reactivity, medication use is one of the most common reasons for unexpected results. Lower-than-expected results are often the result of medication use. Medications that can decrease IgG levels or reactivity include antihistamines, anti-inflammatories (steroids, NSAIDs), anti-cancer agents (alkylating agents, antimetabolic agents, anti-lymphocytic agents, cyclophosphamide, cyclosporine, etc.), and anti-convulsive medications (phenytoins). The use of immunosuppressants and/or antihistamines is contraindicated during allergy testing, and can suppress IgG, and other Ig results. If possible, such medications should be discontinued with the permission of the prescribing physician.
While it is easy to calculate clearance based upon a medication’s half-life, clearance rates do not take into account the recovery time required by the immune system when medications are discontinued. IgG reactivity, signaling pathways, and synthesis rate (minimum four weeks) must all be taken into consideration when patients are using anti-inflammatory or immunosuppressant medications. Human studies regarding the long-term effects of immunosuppressant medications are rare but there is evidence that long-term high-dose oral corticosteroids may dysregulate the immune system for up to 3 years after discontinuation. This may also be true for other types of immunosuppressants, but studies have yet to be done.
There are many different reasons for unexpected IgG results. Pre-analytical errors, which are outside of laboratory control, are responsible for the majority of our unexpected laboratory results. Increased clinician awareness, and improved sample collection education for support staff and patients, can improve collection techniques and sample quality and increase the number of viable results returned to each clinic.
Join us on July 22nd, 2021 for a webinar as we make sense of unusual IgG results and what they may mean for your patients/clients.
Agarwal S, Cunningham-Rundles C. Assessment and clinical interpretation of reduced IgG values. Ann Allergy Asthma Immunol. 2007 Sep;99(3):281-3.
Arul P, Pushparaj M, Pandian K, Chennimalai L, Rajendran K, Selvaraj E, Masilamani S. Prevalence and types of preanalytical error in hematology laboratory of a tertiary care hospital in South India. J Lab Physicians. 2018 Apr-Jun;10(2):237-240.
Cai C, Shen J, Zhao D, Qiao Y, Xu A, Jin S, Ran Z, Zheng Q. Serological investigation of food specific immunoglobulin G antibodies in patients with inflammatory bowel diseases. PLoS One. 2014 Nov 13;9(11):e112154.
Foster AP, Knowles TG, Moore AH, Cousins PD, Day MJ, Hall EJ. Serum IgE and IgG responses to food antigens in normal and atopic dogs, and dogs with gastrointestinal disease. Vet Immunol Immunopathol. 2003 May 12;92(3-4):113-24.
Honma K, Kohno Y, Saito K, Shimojo N, Tsunoo H, Niimi H. Specificities of IgE, IgG and IgA antibodies to ovalbumin. Comparison of binding activities to denatured ovalbumin or ovalbumin fragments of IgE antibodies with those of IgG or IgA antibodies. Int Arch Allergy Immunol. 1994;103(1):28-35.
Leffler D, Schuppan D, Pallav K, Najarian R, Goldsmith JD, Hansen J, Kabbani T, Dennis M, Kelly CP. Kinetics of the histological, serological and symptomatic responses to gluten challenge in adults with coeliac disease. Gut. 2013 Jul;62(7):996-1004.
Nicolaides NC, Pavlaki AN, Alexandra M, Chrousos GP. (2018) Glucocorticoid Therapy and Adrenal Suppression. Endotext https://www.ncbi.nlm.nih.gov/books/NBK279156/ . Accessed 14 June 2021.
Plebani M. Quality indicators to detect pre-analytical errors in laboratory testing. Clin Biochem Rev. 2012 Aug;33(3):85-8.
Overview Many clinicians searching for answers about mycotoxin testing ask questions like “Should I provoke mycotoxins before urine testing?”, “When...

US BioTek Laboratories today announced the completion of its merger with NutriPATH Pathology, a respected functional pathology laboratory serving...

Unlocking the Secrets of Cellular Energy